|
In general, a prolonged QRS from a drug known to cause sodium channel blockade is treated with sodium bicarbonate at a rate of 1-2meq/kg as an initial bolus, followed by a drop of 150 met in 1L D5W at twice maintenance. Overdose treatment for sodium channel blockade may vary slightly depending upon the specific xenobiotic that is causing toxicity. Drugs that block this channel include lidocaine, procainamide, and flecainide. This finding is a result of sodium channel blocker’s preference for blocking the right bundle of the bundle of Hiss (Yates & Manini 2012). There is also a classic ECG finding of a prominent r-wave and a rightward axis of the terminal deflection of the r-wave that is seen in lead aVR of a 12-lead ECG. Sodium channels are responsible for depolarization of myocytes in the atria and ventricles, so blockade of these channels will lead to prolong depolarization and widen the QRS complex (Nelson et al. Calcium channel blockers toxicity can also be treated with calcium itself (3mg/kg/min of CaCl2) (Reikeras et al. This key difference may clue you to a calcium channel blocker overdose in a bradycardia patient.Ĭommon treatment for both beta blockers are calcium channel blockers include high dose insulin and glucose, pressors, glucagon, and phosphodiesterase inhibitors. Calcium channel blockerĬalcium channel blockers (such as amlodipine, nifedipine, diltiazem, verapamil) have similar effects to beta blockers (lower heart rate), but calcium channel also usually block sodium channels, causing conduction delays and QRS widening. 2004), and fat emulsion are also possible treatment options, but only have animal trials or case reports to support their use, so it is unclear if these actually work. 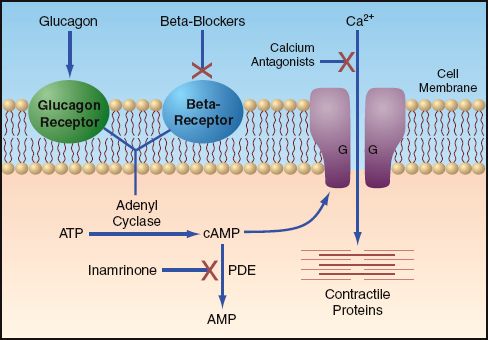
2007), levosimendan (Archan & Toller 2008), pyruvate (Hermann et al. Additionally, phosphodiesterase inhibitors (inamrinone, milrinone, enoximone) can help prevent cAMP breakdown and thereby increase calcium activity within the cell to increase frequency and strength of contract (Nelson et al. Glucagon is the classic first line treatment for beta blocker overdose, but has high rates of vomiting and requires large doses, so most hospitals will exhaust their supply before the beta blocker has time to wear off (Nelson et al. If this fails to correct the hypotension, beta-selective pressers such as dobutamine and isoproterenol may help, but carry the risk of paroxysmal hypotension due to the high doses that are often required (Nelson et al. Hypoglycemia is coming in these patients, so make sure that highly concentrated (≥5% dextrose solutions) glucose is given before the insulin. High dose insulin therapy (1U/kg/hr) with high dose glucose (0.5g/kg/hr) is thought by some to be first line for beta blocker overdose (Nelson et al. There are a few main-stays of treatment, all of which try to counteract the drugs activity at the cell. This leads to low heart rate and blood pressure, as well as an increased probability of sinus bradycardia on ECG. Beta Blockerīeta blockers (such as metoprolol, propranolol, carvedilol) interfere with catecholamine effect on beta adrenergic receptors (principally Beta-1 on heart muscle cells) leading to a decreased heart rate and contractility (Yates & Manini 2012). Luckily, there are some classic ECG changes that will help clue to into what a patient may have overdosed on. You know something is wrong, and a quick review of his nursing home paper work gives you the answer: digoxin toxicity.įiguring out what medication is causing problem for an altered patient can be challenging for any physician.  
Dry mucus membranes, mumbling to himself and not making sense, not responding to your questions, febrile, diaphoretic. You walk back to triage with the tech to see a 86 year old male patient who looks unwell.
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
